There’s more to say (AND DO!) after RU OK?
Today is RU OK Day here in Australia (and World Suicide Prevention Day). This year I was delighted to see in the marketing campaign additional encouragement and support about what to say next if someone isn’t feeling well.
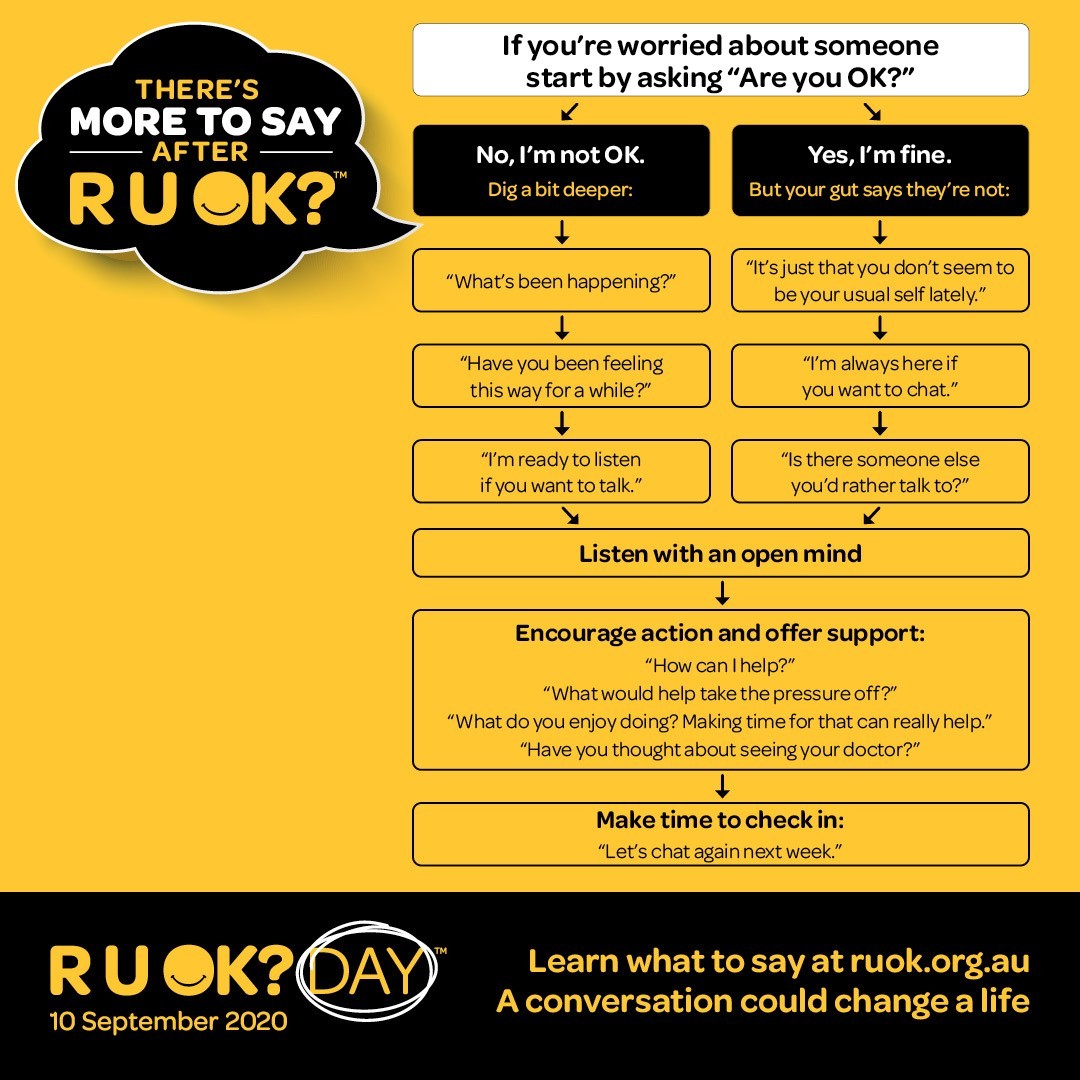
The video above has some great examples of the little things we can all do not just today but any day: “I’m here to listen” or “What can I do right now to support you?”. Another suggestion is to talk to your doctor or seek support.
The focus on action beyond a conversation is extremely important if we’re going to reduce the significant mental health burden here in Australia and globally.
Checking in with your GP really is the first stop if you’re concerned about your mental health. Your GP can rule out other potential physiological or biological issues that may be affecting your mental health. Once they’re ruled out, the next step is to seek professional psychological or psychiatric support. Although I still hear from many people that they haven’t been referred on and this concerns me. Many GPs spend countless hours counselling their patients around mental health issues. While that’s part of building a strong doctor-patient relationship, in many cases a referral to a mental health professional is required – which may be in addition to medication, or as a primary intervention.
And yes it does cost money in most cases to seek professional assistance – as it does with other professional services we seek such as lawyers and accountants – and while there are Medicare rebates available, not all psychologists or psychiatrists bulk bill.
However, there are other mental health services available that your GP should make you aware of eg Headspace. You can also do a google search on free mental health services in your community. Universities with psychologists in training often provide services at significantly reduced rates.
So while I hear that cost is a factor, I often muse that people don’t hesitate to spend money on other items or experiences to feel good or well, or are happy to have their car serviced annually, but they often hesitate or procrastinate on spending money on a “mental health check-up” or extended therapy and use this as an excuse for not seeking help.
I spent over 15 years working as a Clinical Psychologist here in Australia and saw hundreds of people with mental health disorders. Some were really struggling with severe psychiatric diagnoses such as schizophrenia or bipolar disorder.
Others were suffering with what’s become known as the common cold of mental illness being depression and/or anxiety. Not everyone was completely healed as a result of seeking assistance, as many people I consulted with were suffering with severe trauma and issues that would require more than 6-10 Medicare funded sessions.
They did however leave our sessions with a set of psychological skills that they could use for the remainder of their lives, regardless of the ups and downs. In fact, it was this realisation, that led me to pursuing a career in the field of Positive Psychology, as a proactive approach to mental health and illness. I realised that most people wait until they’re unwell before they seek psychological support.
For the past 15 years I’ve been firmly focused on educating people on proactive mental health and wellbeing and teaching key psychological capabilities through workshops, webinars, courses and leadership and personal coaching.
Over the years, it has been good to see the stigma of seeking psychological help has reduced somewhat however I think we’ve got a long way to go. Here in Aus, it’s not like we brag about our therapists like they do at dinner parties in New York City! I recall reading a twitter post a while back where an Australian journalist reflected on a recent dinner party she’d attended. She innocently asked the question at the dinner table “Can anyone recommend a great therapist?” and she noted there was dead silence – you could hear a pin drop!
This year, keep asking R U OK but be sure to talk about the benefits of seeking professional assistance. Talk about your own experience with counselling or therapy, if you’ve been, or perhaps the experience of a friends or family member. While you’re likely to hear responses such as “I’ve tried that, didn’t work” or “Not for me”, you’re also likely to hear “Best thing I ever did!” and “Why did I wait so long to get help!”.
Of course, like finding any good professional, you need to do your homework and be prepared to find another therapist if you think it’s not a good fit. In fact, research has shown that the “therapeutic alliance” or “working alliance” is a reliable predictor of outcomes. That is simply, how well you and your therapist work together – your bond – and how well you agree on the goals and tasks of therapy. So, if you’ve been once and are one of the hundreds, perhaps millions of people here in Australia, that haven’t been back, I’d encourage you to try again – and again – if you need. And if you’ve never been, making the decision to go, may save your life.
So today, do ask “RU OK?” Recommend action such as seeing the GP and a mental health professional. But also remember to ask at the next dinner party you attend – “Do you know a good therapist?” Life’s too short to languish.
Post
